Information for Geneticists and Genetic Counsellors about Malignant Hyperthermia (MH)
MH is a potentially life-threatening condition which is avoidable if anaesthesia is given with no triggering agents.
Some MH susceptible individuals present outside of the operating theatre. Known associations with MH susceptibility are exertional rhabdomyolysis, hyperCKaemia, exertional heat illness, central core disease and multiminicore myopathy. There are also rare reports of MH susceptible individuals who present with episodes of fever and muscle rigidity unrelated to drug exposure that can prove fatal.
There is evidence that MH susceptibility is one of a growing number of presumed single gene disorders that deviates from a simple Mendelian model of inheritance. Indeed, inheritance of MH can be best explained by a threshold model: many MH families appear to have more than one genetic factor making a major contribution to the risk of MH susceptibility.
MHANZ member laboratories (all of whom follow the EMHG testing guidelines) offer an in-vitro contracture test (IVCT) to family members who test negative for the family mutation.
MHANZ is conservative with interpreting predictive genetic tests. MHANZ recognises many families that have discordance between genotype and phenotype suggesting the presence of a second mutation or a modifying variant.
As a result genetic diagnosis of MH with the presence of a known causative mutation is possible but the converse is not true.
The only way to rule out MH is with a biopsy, absence of the family mutation is not an adequate test for non-susceptibility.
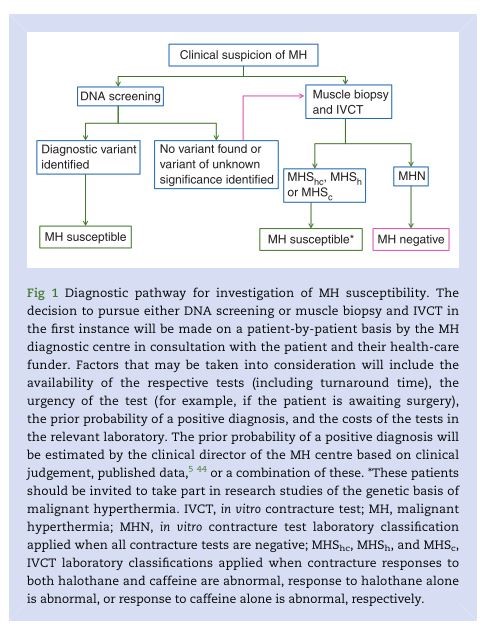
For patient safety, individuals carrying a potentially a potentially MH causative RYR1 variant should be regarded at increased risk for MH until further diagnostic tests, i.e., an IVCT, have been performed.
Many RYR1 variants have been found in MH and non-MH susceptible individuals. The EMHG has developed a scoring matrix for pathogenicity prediction http://www.emhg.org/genetics
Genetic testing for MH should be done in consultation with an MH Diagnostic Unit.
1. Hopkins PM RH, Snoeck MM, Girard T, Glahn KPE, Ellis FR, Müller CR, Urwyler A on behalf of the European Malignant Hyperthermia Group. The European Malignant Hyperthermia Group guidelines for the investigation of malignant hyperthermia susceptibility. Br J Anaesth 2015; 115: 531-9